Process
This project started with a question: “How can Service Design help cancer survivors and their loved ones to improve their cancer experience and quality of life?” The focus was understanding the current cancer experience; survivors’ and their loved ones’ needs and wants were key to finding solutions. This project visualized the entire journey of the high-level cancer experience with a Cancer Experience Map (CEM) and created a Desired Survivorship Experience Framework (DSEF) to empower service designers and healthcare providers to work together, generate new ideas and bring more comforting services, as well as validate and evaluate existing ideas, to improve the lives of survivors, their families and friends.
1. In-depth Interviews
Thirty-one stakeholder interviews and two expert interviews were conducted from March to July 2015. These interviews provided a deeper understanding of cancer survivors’ and their loved ones’ needs and wants, as well as perspectives from experts with years of specialized experience in healthcare design and caring for cancer survivors, their families, and friends.
2. In Context Immersion
Immersing myself in the context to meet survivors where they live, work, and socialize revealed new insights and unexpected opportunities. I spent several days joining survivors’ support group meetings. This allowed me to see survivors’ perspectives and gain true empathy through being with them in their real-life settings and doing what they normally do such as volunteering at a cancer race event. These immersion activities provided this project with informed intuition that was applied to research insights and future design.
3. Co-creation Activities
10+ co-creation session and workshops were conducted during different phases of this project based on different needs and goals in each phase. One of the main objectives was to explore and co-create a CEM to bring in clarity from various stakeholders to understand what the current cancer experience looks like and gather a broad range of perspectives in the process. Many of these sessions were conducted at the Curtis & Elizabeth Anderson Cancer Institute at Memorial Health University Medical Center. These workshops also provided opportunities to engage different stakeholders in a series of conversations about the topic with prominent healthcare practitioners.
A 160-inch long by 45-inch wide CEM was co-created with social workers, nurses, other hospital staff and caregivers during these sessions and workshops. It identified high-stress points, patients’ energy level changes, emotional changes, different potential pathways based on each decision-making point, and various relationships and interactions among stakeholders within each step throughout the whole cancer journey.
4. Analyzing, synthesizing data and identifying patterns and themes
1500+ data points were collected and sorted. Patterns and themes were identified through the process. The affinity diagram shows that nine common themes emerged from the research, revealing insights that some stakeholders like healthcare providers were notaware of, such as why some survivors knew there was help available but wouldn’t take advantage of it.
5. Translating Insights
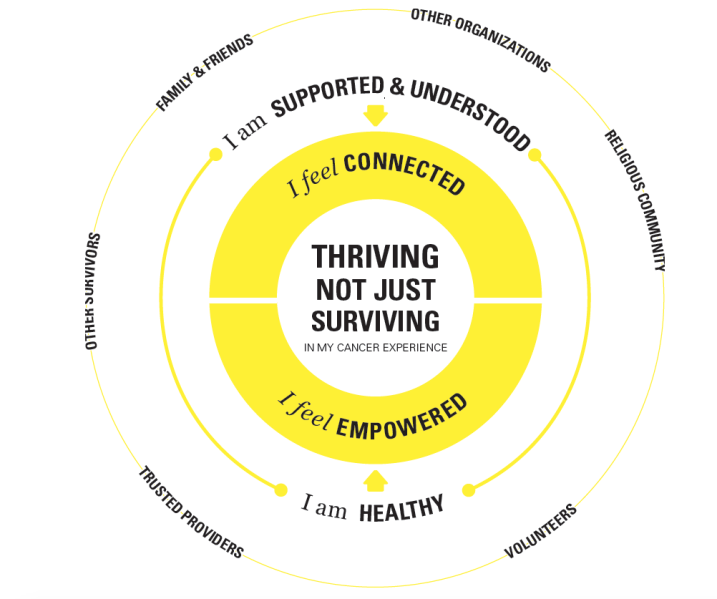
Insights gathered from the research were translated into a DSEF, a tool that facilitates communication, awareness, and innovation in cancer care. It is grounded in engaging, actionable insights from the voice of cancer survivors, enabling service designers to view the current issue from an alternative perspective and work together toward a desired future vision.
6. Prototyping and Testing
The DSEF was presented and tested within the design community for critique. The workshop was conducted with service designers to refine and improve the framework. 80+ service concepts were generated by using the framework. User pain points were quickly identified, addressed and incorporated into the final solution.
Output
Two main outcomes of the project are the Cancer Experience Map (CEM) and the Desired Survivorship Experience Framework (DSEF).










Share your thoughts
0 RepliesPlease login to comment