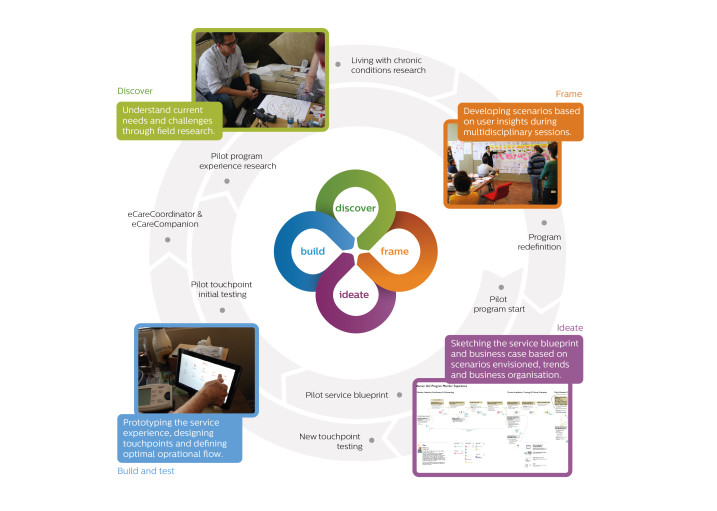
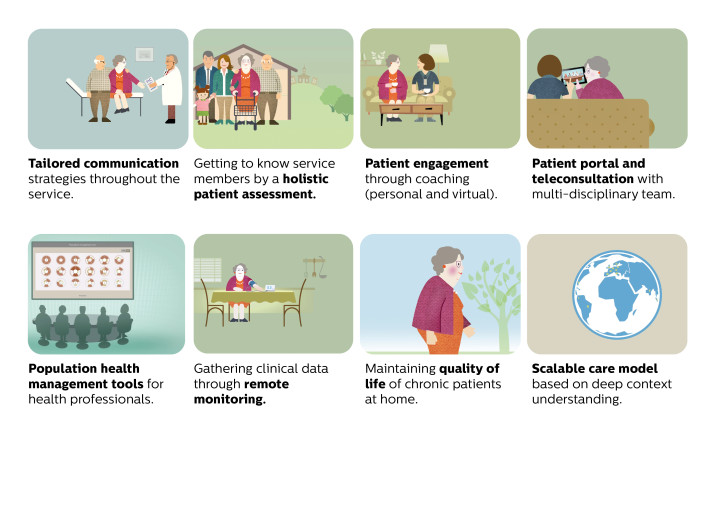
One of the biggest challenges for healthcare organizations is to deliver care to patients with multiple chronic conditions. In addition to being the most challenging population to manage, they also are the costliest. While they make up only 5% of patients, they account for up to 50% of all healthcare spending. Focusing on the most complex and highest cost patients, the eIAC program (Intensive Ambulatory Care) is designed to support chronically ill patients to manage their condition at home. The eIAC program enables all stakeholders in the clinical and social management of a patient to identify and address the root causes of the patient’s frequent admissions. This creation of a cohesive system of care will help to reduce hospital admissions while providing the highest level of care to patients with complex, and multiple chronic conditions. The eIAC service proposition combines leading telehealth technologies that monitor and educate patients with a patient portal (eCare Companion patient app). This transformed clinical model unites former factionalized care team members by using the eCare Coordinator software platform to enable clinicians to remotely monitor patients and make informed and timely decisions. The program enables the transition to patient-centered, cost-effective, proactive health management while supporting pay-for-value care delivery.

Join us at SDGC26 - registration is open
Connect, Collaborate, and Create Change – SDGC26 Awaits! Join us in Wiesbaden, Germany and online, 28–30 October. Registration is open.







Share your thoughts
0 RepliesPlease login to comment